Metabolic
Syndrome Is a Risk after Liver Transplantation, Leading
to Poor Outcomes
 |
 |
 |
 |
 |
 |
 |
| SUMMARY:
As people survive longer after liver transplants,
the development of metabolic syndrome is
a growing concern -- an epidemic waiting
to happen -- according to a review article
published in the December
2009 issue of Liver Transplantation.
Studies indicate that diabetes, hypertension,
and other manifestations of the syndrome
are more common in liver transplant recipient
than in similar non-transplant patients.
These conditions increase the risk of cardiovascular
disease, and indicate the need for better
management including lifestyle modifications
and lipid-lowering drugs. |
|
 |
 |
 |
 |
 |
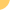 |
 |
By
Liz Highleyman
Over
years or decades, chronic
hepatitis B or C
infection can progress to advanced liver damage
that necessitates a transplant. As post-transplant
survival has improved, metabolic syndrome and its
individual components -- including diabetes mellitus,
hypertension, dyslipidemia (abnormal blood fat levels),
and obesity -- are increasingly recognized as a contributor
to cardiovascular complications and late morbidity
and mortality, wrote Mangesh Pagadala and colleagues
from the Digestive Disease Institute of the Cleveland
Clinic Foundation.
The
prevalence of post-transplant metabolic syndrome and
its components has been found to be higher in transplant
recipients (43%-58% after 12 to 18 months) compared
with an otherwise comparable population who do not
receive transplants (about 25%). The development of
nonalcoholic fatty liver disease (NAFLD) after liver
transplantation (for reasons other than non-NAFLD
cirrhosis) is also increasingly recognized.
Most patients with liver disease severe enough to
require a transplant have some degree of insulin resistance,
and this typically improves after transplantation.
Persistent or newly emerging insulin resistance post-transplantation,
however, is a cause for concern.
Several potential pre-transplant risk factors for
post-transplant metabolic syndrome have been identified,
including older age, male sex, history of smoking,
higher pre-transplant body mass index (of the liver
recipient or donor), and pre-transplant diabetes.
Patients who receive transplants due to hepatitis
C, alcoholic cirrhosis, or cryptogenic (unknown cause)
cirrhosis are also at higher risk. Another risk factor
is immunosuppression, caused by drugs used to prevent
organ rejection (also suggesting potential concern
for people with HIV).
Patients with post-transplant metabolic syndrome have
an increased risk of cardiovascular events, organ
rejection, and all types of infection, the researchers
noted. According to one study, the risk of cardiovascular
events was about 30% among people who developed post-transplant
metabolic syndrome, compared with 8% among people
who did not. However, the overall impact of metabolic
syndrome on long-term survival and mortality remains
to be determined.
Strategies to reduce the development of metabolic
syndrome -- both before and after transplantation
-- should include lifestyle modifications involving
improved diet, increased physical activity, and weight
loss, they concluded. Additional measures that may
be beneficial include use of lipid-lowering medications,
optimal blood glucose control, and use of tacrolimus
instead of cyclosporine for immune suppression.
Department of Gastroenterology & Hepatology
and Department of Hepatobiliary Surgery, Digestive
Disease Institute, Cleveland Clinic Foundation, Cleveland,
OH.
1/15/10
Reference
M Pagadala, S Dasarathy, B Eghtesad, and AJ McCullough.
Posttransplant metabolic syndrome: an epidemic waiting
to happen. Liver Transplantation 15(12): 1662-1670
(Abstract).
December 2009.