Rapid
Liver Fibrosis Progression and Successful Treatment of Acute
Infection Suggest Benefits of Routine HCV Screening for
HIV Positive Men
 |
 |
 |
 |
 |
 |
 |
| SUMMARY:
Researchers from Mt. Sinai School of Medicine
presented data last week at the 60th Annual Meeting
of the American Association for the Study of Liver
Diseases (AASLD) in
Boston that further characterize a cohort of HIV
positive men with apparently sexually transmitted
acute hepatitis
C virus (HCV) infection. This group continues
to experience more rapid than expected liver
fibrosis progression. Hepatitis
C treatment has been highly successful if
started during the acute phase, but less so thereafter.
The researchers recommended routine ALT and HCV
antibody testing to allow for prompt treatment
and to prevent liver disease progression. |
|
 |
 |
 |
 |
 |
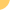 |
 |
By
Liz Highleyman
Starting
around 2002, clinicians in large cities in the U.K. and
Europe began reporting outbreaks of acute HCV infection
among HIV positive gay and bisexual men, which were associated
with sexual risk factors and reflected social and sexual
networks. Such outbreaks have since been reported in Australia
and the U.S.
Dr.
Daniel Fierer and colleagues have been following a cohort
of HIV/HCV coinfected men seen at Mt. Sinai in New York
City. They first
reported on rapid fibrosis progression in this group
at the Conference on Retroviruses and Opportunistic Infections
(CROI) in 2007, following up with data
from the growing cohort at CROI 2008 and CROI
2009, and in the September
1, 2008 Journal of Infectious Diseases.
This
year at AASLD, Dr. Fierer presented
data from 51 HIV positive men who have sex with men (MSM)
who experienced 53 episodes of acute hepatitis C (some were
infected twice). Acute HCV infection was defined as newly
identified HCV antibody seroconversion, marked elevation
in liver function tests (ALT > 5 times the upper limit
of normal), or large fluctuations in HCV RNA level (>1
log in 4 weeks).
|
ACUTE
HEPATITIS C
|
 |
The
median age of the coinfected cohort was 40 years. About
half (27 men) were white, 17 were Hispanic, 6 were black,
and 1 was Asian. Most (49 men) had HCV genotype 1. The median
duration of HIV infection was 7 years (range 0 to 20 year)
and the median CD4 cell count was 471 cells/mm3; 14 men
-- 27% of the cohort -- had never received antiretroviral
therapy for HIV.
Out
of this group, 21 patients and 21 age-matched HIV positive
but HCV uninfected men were included in a case-control analysis
to identify sexual and drug use risk factors for acute HCV
infection. In addition, 30 of the coinfected men underwent
liver biopsy histology evaluation (median 4.4 months after
their first ALT elevation) and 34 were treated with pegylated
interferon plus ribavirin.
Results
 |
Spontaneous
HCV clearance occurred in only 5 cases (9%), with 3
still under evaluation. |
 |
In
the case-control study of 21 matched pairs, the factors
significantly associated with increaed risk of HCV infection
were: |
 |
Unprotected
receptive anal intercourse with ejaculation (P
= 0.04); |
 |
Unprotected
receptive anal intercourse without ejaculation
(P = 0.03); |
 |
Unprotected
receptive oral sex with ejaculation (P = 0.03);
|
 |
Use
of sex toys (P = 0.03); |
 |
Sex
while "high" (P = 0.01); |
 |
Marijuana
use (P = 0.04). |
|
 |
Protected
receptive anal intercourse, protected receptive oral
sex, and fisting -- risk factors reported in some other
HIV positive MSM coinfection cohorts -- were not significantly
associated with acute HCV infection (all P > 0.05). |
 |
The
traditional risk factors of injection drug use and sharing
injection equipment also were not significantly linked
to HCV infection (again, all P > 0.05). |
 |
Among
the treated patients: |
 |
1
was lost to follow-up; |
 |
15
were still receiving therapy; |
 |
16
were assessed for sustained virological response
(SVR) 24 weeks after completing treatment; |
 |
1
achieved an end-of-treatment response and was
pending further follow-up to assess SVR. |
|
 |
Of
the 16 patients who completed therapy and were evaluated
for SVR: |
 |
12
(75%) achieved a sustained response. |
 |
1
never suppressed HCV RNA; |
 |
2
responded but experienced viral breakthrough during
treatment; |
 |
1
achieved virological response but relapsed after
completing treatment. |
|
 |
3
of the 4 patients who did not achieve SVR started treatment
after the acute phase (i.e., more than 6 months after
their first ALT elevation). |
 |
Among
the 30 participants who underwent liver biopsies: |
 |
21
(70%) had stage 2 (moderate) fibrosis using the
Scheuer scale (0 to 4); |
 |
2
(7%) had stage 3 (advanced) fibrosis; |
 |
5
(17%) had stage 1 (mild) fibrosis; |
 |
2
(7%) had stage 0 (absent) fibrosis. |
|
 |
77%
participants had fibrosis stage > 2 at this
phase of infection, while just 24% had stage < 2. |
 |
Fibrosis
stage increased with time-to-biopsy; of the 7 biopsies
performed more than 1 year after the first ALT elevation,
all showed stage > 2 fibrosis. |
These
findings indicate poorer outcomes among individuals who
are already HIV positive at the time of acute HCV infection.
The spontaneous clearance rate of 9% is considerable lower
than the approximately 25% reported in most studies of HIV
negative people. Furthermore, the extent of liver damage
during acute or early infection was dramatically greater
than that observed in most studies of HIV negative patients.
One such study, for example, found that all 87 patients
assessed during acute infection had stage 0 fibrosis, with
none having stage 1 or higher.
Participants
in the Mt. Sinai study had none of the usual risk factors
associated with pre-existing liver fibrosis, including a
history of ALT elevation or heavy alcohol use. Hepatitis
B triple infection was rare. Most had a healthy body weight
and normal blood sugar levels. One-quarter had never taken
antiretroviral drugs and some reported never using any recreational
drugs.
Based
on these findings, the researchers concluded that acute
HCV infection of HIV positive MSM in New York City is sexually
transmitted and results in "rapid and significant"
liver fibrosis progression. They added that acute HCV infection
was associated with unprotected receptive sex.
"This
epidemic represents a new clinical syndrome for HCV infection
that turns much of our knowledge on its ear," Dr. Fierer
said in a press release issued by AASLD. This is "a
new risk group becoming infected through a previously rare
route of transmission resulting in unprecedented progression
of liver fibrosis."
"Treatment
is highly successful when initiated in the acute phase,
but may be less successful if initiated soon after,"
the investigators noted. "Thus, it is crucial to detect
HCV infection in the acute phase to allow successful treatment
and prevent further progression of the already significant
liver fibrosis."
"We
therefore recommend ALT testing every 3 months and HCV antibody
testing every 6-12 months for all HIV-infected MSM,"
they advised. "Promotion of safe sex is also warranted."
Department
of Medicine and Department of Pathology, Mount Sinai School
of Medicine, New York, NY.
11/10/09
Reference
DS Fierer, AJ Uriel, DC Carriero, and others. Characterization
of an Epidemic of Sexually-transmitted Acute Hepatitis C
Infection in HIV-infected Men in New York City. 60th Annual
Meeting of the American Association for the Study of Liver
Diseases (AASLD 2009). Boston. October 30-November 1, 2009.
Abstract 82.
Other
source
AASLD.
New
Epidemic of Sexually Transmitted Hepatitis C Infection in
HIV-infected Men in NYC. Press release. October
30, 2009.